Tag: healthcare
-
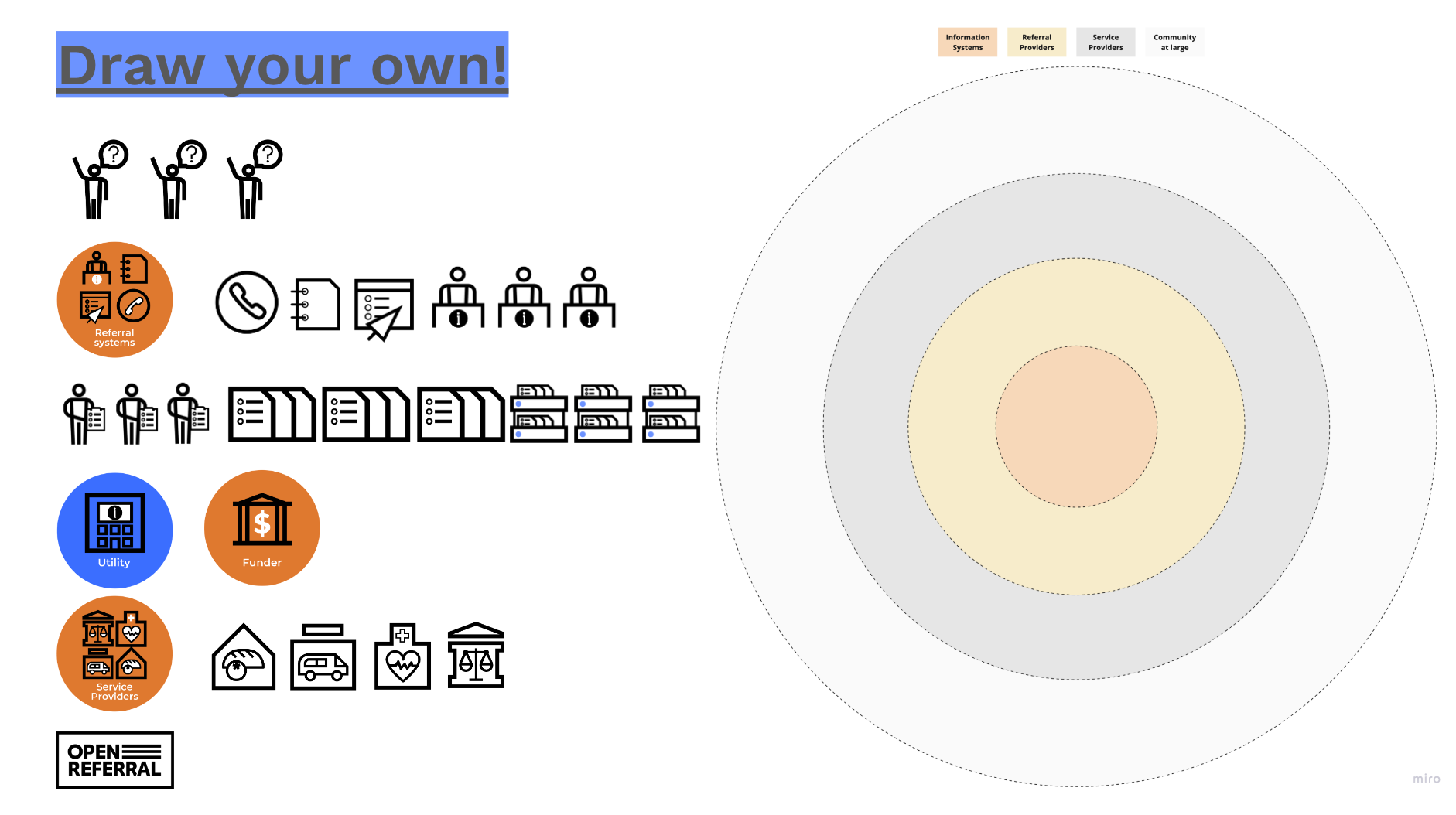
Envisioning cooperative resource directory information infrastructure in Minnesota
Minnesota residents can look for information about a range of human services on MinnesotaHelp.Info®, a resource navigation program supported through partnership among several public entities (including the state’s Department of Human Services and Board on Aging). Minnesotans can also look for information about human services via 2-1-1, which is operated by United Ways of Minnesota…
-

Resource data as a service: 2-1-1 Maryland’s new integration with their state’s healthcare IT infrastructure
We’ve partnered with 2-1-1 Maryland over many years, so we’re especially proud of their recent partnership with CRISP – Maryland’s Health Information Exchange – and Maryland’s Department of Health. This year, we helped 211MD and CRISP develop a groundbreaking partnership with MDH’s Primary Care Program. The results of this partnership point to exciting new horizons…
-
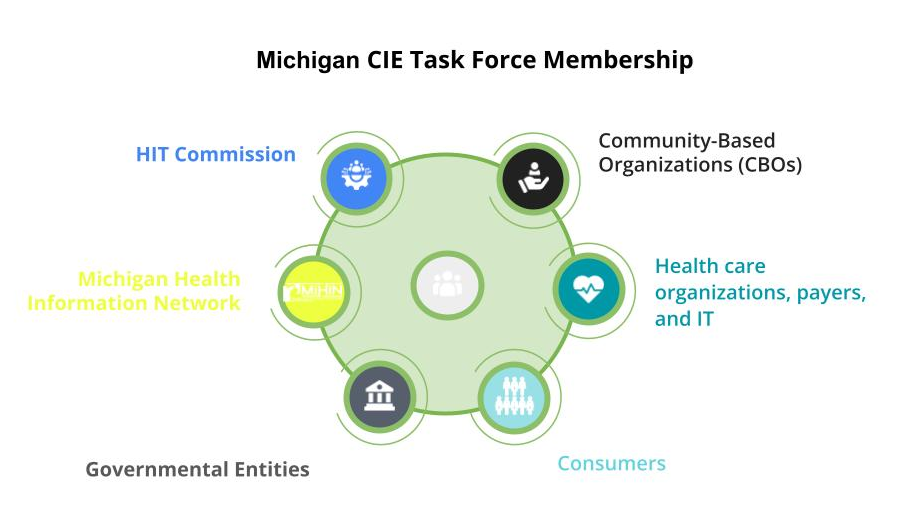
The Community Information Exchange Task Force Report from Michigan’s Dept of Health and Human Services
I’ve had the honor and privilege of working with the Michigan Community Information Exchange Task Force over the past year. I encourage you to read the report, which is published here. You can also watch this webinar summarizing the report with commentary from a range of task force members. In my (admittedly biased) opinion, this…
-

HSDS is now interoperable with FHIR®
As integration of healthcare and social care sectors becomes an ever-hotter topic, we’re excited to announce that we’ve taken a small but significant step forward: the Human Service Data Specifications are now aligned with the protocols for healthcare provider directory information specified by the Health Level Seven (HL7®) Fast Healthcare Interoperability Resources (FHIR®).
-

Laying the foundation for a community information exchange in Utah
In 2021, Utah’s incoming governor Spencer Cox outlined a plan – the One Utah Roadmap – to address key priorities for the state in his first 500 days, ranging from coordinated COVID response to addressing the social determinants of health. In support of these priorities, the Governor’s office formed a working group focused on the…
-
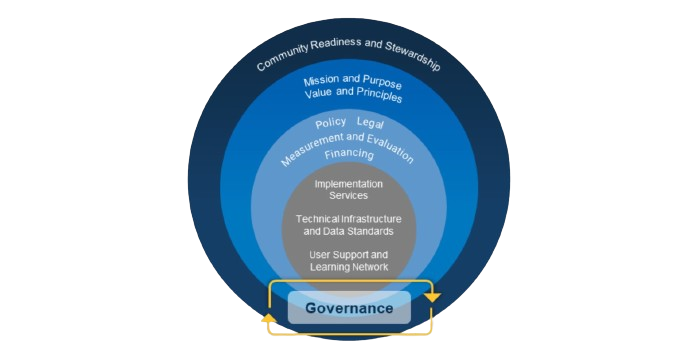
Just Released: Toolkit for information exchange initiatives from the Office of the National Coordinator of Health IT at HHS
I’m excited to share with you this toolkit for information exchange initiatives that aim to address the social determinants of health – shared by the Office of the National Coordination for Health Information Technology at the US Department of Health and Human Services (known as ONC). The toolkit (PDF downloadable here) synthesizes subject matter expertise…
-
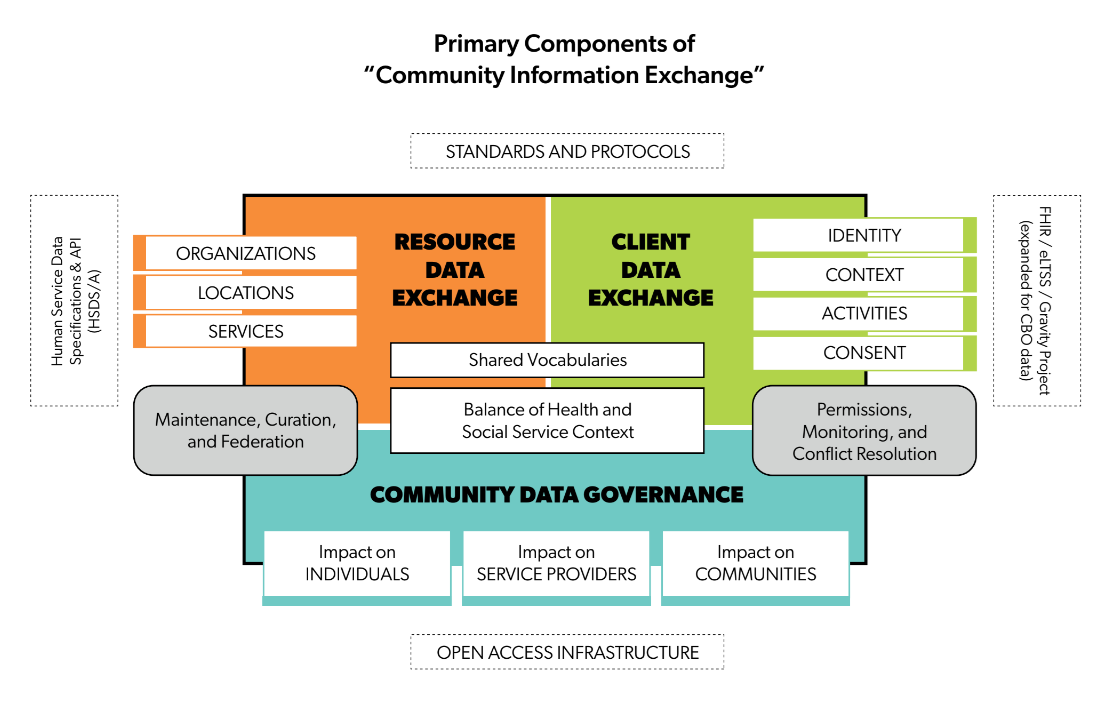
Tackling Data Dilemmas in Social Care Coordination: A Whitepaper on Community Information Exchange
Last year – with sponsorship from Robert Wood Johnson Foundations’ DASH program, and in partnership with the Regional Data Alliance at University of Missouri St Louis – I co-authored a whitepaper that aggregated research and recommendations from across the emerging field of “social care coordination.” This paper provides a strategic framework in which to understand…
-

Supporting the Gravity Project to expand interoperability among health, human, and social services
Often people ask how we enable care providers to actually refer their clients to another service. The answer is, well, Open Referral doesn’t actually deal with the process of “making a referral” at all! We’re working to ensure that there’s open access to information about the services to which someone might be referred. But the…
-

Innovating Around the Intervention: Activate Care’s Coordination Tools, Powered by Open Referral
[Welcome to Jonathan Abbett, VP of User Experience at Activate Care!] Imagine if our healthcare and social service systems were able to seamlessly coordinate care around all of our physical, behavioral, and social health needs. Back in 2012, inspired by this vision, I joined a technology start-up that is now known as Activate Care. I…
